Onychomycosis (Fungal Toenails)
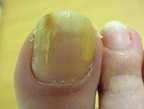
What is Onychomycosis?
Onychomycosis (also known as tinea unguium) is a contagious fungal infection of the toe nails that affects about 6-8% of the adult population. Fungal infection in the toe nails account for almost half of all nails problems, with its incidence increasing with age. These fungal infections can occur when one of a number of types of microscopic fungi gain entry (usually through minor trauma) to the nail, then grow and spread in the warm, moist environment inside socks and shoes.
Symptoms
Usual symptoms involve changes in the appearance of the nail. This can include swelling, yellowing, thickening, roughness, or crumbling of the nail, streaks or spots down the side of the nail, and even complete loss of the nail. Toenail colour can vary from brown to yellow or white. Yellow to brown coloured nails may also have a strange odor noted when they are cut
Generally, fungal nails are not painful, though chronic infected nails can change shape and then cause other painful nail conditions.
Cause
Onychomycosis is caused by fungal organisms such as: dermatophytes, Candida (yeast) and non-dermatophyte moulds. In Adelaide and the lower states of Australia, onychomycosis is predominately caused by Dermatophytes. In upper Queensland and in the tropics, Candida and non-dermatophyte moulds are more commonly involved as the cause.
Toenail fungus is often picked up in damp areas such as public gyms, showers and swimming pools as the dermatophytes thrive in warm damp areas. In many cases, it’s not just the nails that can catch fungal infections as the fungi often spreads from the skin to the nails and vice versa.
Factors that may lead to developing onychomycosis include:
- Trauma that allows the pathogen to enter the nail or nail bed
- Abnormal PH level of the skin,
- Not drying off the feet thoroughly after bathing or exercise
- Wearing tight, or enclosed shoes that do not allow feet to breath.
- Diabetics and the elderly have an increased risk of contracting a toenail fungus because their immune system is compromised. For this reason it is often recommended that they should have their nails cut and callus debrided by a podiatrist.
Types of Onychomycosis include:
Distal subungual onychomycosis: The most common form onychomycosis that invades the nail bed and the underside of the nail plate from the tips down. These fungal infections are often yellow brownish in colour and include most of the symptoms above including thickening, roughness, or crumbling of the nail, streaks or spots down the side of the nail, and even complete loss of the nail.
White superficial onychomycosis: this type of fungal infection occurs on the outer most surface of the nail and often appears as white spots. It is one of the easiest types of infections to treat accounting for only 10% of all cases of onychomycosis.
Proximal subungual onychomycosis: this type of infection occurs in the area of new nail growth at the beginning of the nail and almost always occurs in people with other health problems (i.e. who are immuno-compromised). It is the least most common type of onychomycosis.
Candidal onychomycosis: this is type of onychomycosis often occur in people who frequently immerse their feet in water. It normally occurs after trauma/damage of the nail that allow the Candida to invade.
Diagnosis
Conformation via culture of nail scrapings or clippings can often be poor. Diagnosis is therefore best made by a qualified podiatrist. Differential diagnosis may include nail psoriasis, contact dermatitis, trauma, lichen planus, nail bed tumour or yellow nail syndrome.
Treatment
Because it is difficult to treat or eradicate toenail fungus, prevention is always better than a cure. If you do develop toenail fungus it is generally advised to see your podiatrist who can remove or file off as much of the infected nail as possible if required and recommend what sort of treatment is best for your type of onychomycosis. In many cases, medicated nail tinctures may be prescribed if the infection is localised. However, if the infection is more serious, your doctor may prescribe oral antifungal medication. These medications can have side effects and should only be given if a positive culture is obtained.
Prevention
- Wear protective shoes or sandals in public showers, pool areas and gyms,
- Avoid borrowing someone else's shoes, sharing socks or towels
- Wash your feet regularly, dry them thoroughly when they get wet.
Note: Wearing nail polish is generally not advised for those suffering from nail fungus, because it seals the fungus in a warm and most environment and may encourage it to grow.
Avoid Nail Salons that re-use their nail cutting instruments or nail files. Instruments should be sterilised using an autoclave.
Keep toenails trimmed, and be sure to disinfect any pedicure tools before using them.
If you suspect that you have toenail fungus, it is generally recommended that you see your podiatrist before it spreads.
Related Stories
Nail Problems
Ingrown toenails
Nail Surgery
Podiatry
Podiatry Pedicures
Contact Us |
Services |
Foot Conditions |
|


